Have you ever been told that you’re a “loud” sleeper? Regular snoring, snorting, or gasping could be signs of sleep apnea, a common disorder in which breathing frequently stops and starts. Although the two often go hand-in-hand, not all snorers have sleep apnea.
a lack of quality sleep can result in various health problems, including obesity, diabetes, hypertension, and heart disease.
Getting a good night’s rest is crucial for mental and physical health. According to the National Institutes of Health, a lack of quality sleep can result in various health problems, including obesity, diabetes, hypertension, and heart disease.
What Causes Sleep Apnea?
There are two main types of sleep apnea, with nearly identical symptoms: Obstructive Sleep Apnea (OSA) and Central Sleep Apnea (CSA).
- Obstructive Sleep Apnea happens in your airway while sleeping and is often associated with snoring. Your airway may narrow, creating limited airflow to breathe, causing your soft tissue to vibrate (snoring), or the airway may collapse, leading your breathing to stop.
- Central Sleep Apnea occurs when the brain does not transmit the signals necessary to breathe.
The American Journal of Respiratory and Critical Care Medicine estimates that more than 22% of all adults ages 18-90 have obstructive sleep apnea alone.

What Are The Symptoms of Obstructive and Central Sleep Apnea?
It’s not uncommon for obstructive and central sleep apnea symptoms to get confused. The most common overlapping symptoms are:
- Loud snoring
- Disruptive breathing episodes during sleep (which would be reported by another person)
- Gasping for air during sleep
- Awakening with a dry mouth or sore throat
- Morning headache
- Difficulty remaining asleep (insomnia)
- Excessive daytime sleepiness (hypersomnia)
- Trouble concentrating
- Heartburn
- Waking up several times a night to urinate
- Irritability
- Sudden shortness of breath or chest pains at night
Individuals with obstructive and central sleep apnea can be unaware of symptoms until observed by a bed partner. If you think you might have either of these sleep disorders, please talk with your healthcare provider.
What Are The Risks?
Experiencing repetitive breathing disruptions throughout sleep creates stress in the body and increases the chances of developing several other health issues. Here are seven risks related to sleep apnea:
- High blood pressure. As a result of stopping breathing, your body attempts to absorb more oxygen, possibly leading to hypertension.
- Heart disease. Untreated sleep apnea increases the risk of irregular heartbeats, coronary heart disease, heart attacks, and congestive heart failure.
- Stroke. When blood flow to the brain is disrupted repeatedly, it often results from a blood clot that blocks arteries or a broken blood vessel, which amplifies stroke risks.
- Brain damage. As a result of inadequate sleep, memory loss, attention problems, and dementia are common.
- Depression. Research shows a direct correlation between sleep, mood, lack of sleep, and depression. Another study found that nearly 46% of people with obstructive sleep apnea had depressive symptoms.
- Diabetes. It can be difficult to manage diabetes with sleep apnea. As a result of the constant stops and starts during sleep, the body can’t use insulin effectively, resulting in insulin resistance.
- Obesity. As energy levels decline during the day, physical activity decreases as well. Sleep apnea plays a role in metabolic functions, and it may alter hormone levels that regulate appetite, leading you to eat more and potentially gain weight.
Constant interruptions reduce sleep quality and, if left untreated, can lead to potentially severe health consequences.
Research shows a direct correlation between sleep, mood, lack of sleep, and depression.
How is Sleep Apnea Diagnosed?
Before completing tests, your doctor will want to rule out any other possible symptoms affecting your sleep. Typical questions include:
- Do you take any medications? Certain medicines can aggravate untreated sleep apnea or become problematic if diagnosed.
- What is your medical history? Health issues can put you at a higher risk of developing a sleep disorder.
- Have you traveled recently? Any altitude higher than 6,000 feet has low oxygen and might trigger sleep apnea symptoms.
Once your doctor finishes this assessment, they will further evaluate you by conducting the following:
- Physical exam. A general exam is one of the best ways to diagnose sleep disorders. Your doctor will:
– Listen to your lungs and heart, and check neurological systems
– Evaluate your jaw structure, size, and position of your tongue
– Look for other conditions that can heighten your risk for sleep apnea, such as obesity, narrowing of the upper airways, enlarged tonsils, or large neck circumference
Depending on your doctor’s findings, they may order additional tests, such as:
- Sleep studies. Your provider may refer you to a sleep specialist or a center for a sleep study. Fortunately, you can complete these studies in the comfort of your home. The tests will:
– Identify disruptions in sleep
– Determine low or high levels of muscle activity that control breathing
– Examine blood oxygen levels
– Monitor heart and brain activity during rest - Blood tests. Your doctor may want to check hormone levels to rule out endocrine disorders that can lead to sleep apnea.
After your test is complete, your doctor will identify if you have mild, moderate, or severe sleep apnea. Individuals with mild sleep apnea typically have 5-14 events in an hour, 15-19 in moderate cases, and in more severe instances, 30 and above in an hour.
Can Sleep Apnea Be Treated?
Suggested treatments are dependent on test results and the severity of your condition. For example, in mild cases, you’ll need to make lifestyle changes, like losing weight, smoking cessation, or treating nasal allergies. In moderate to severe cases of sleep apnea, other treatments include:
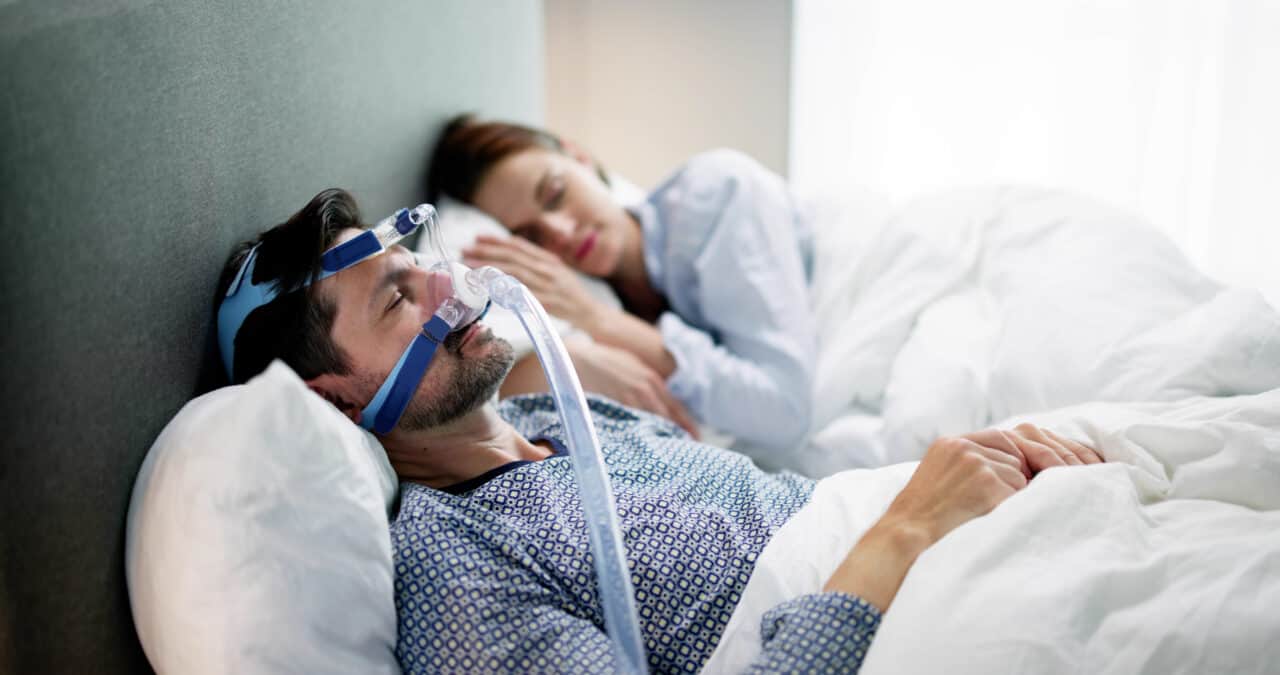
- Continuous Positive Airway Pressure Machine (CPAP). Air pressure is transferred through a mask while you’re asleep, opening the upper airways, which can eliminate sleep apnea and snoring.
- Oral appliances. Mouth guards and mandibular advancement devices are available to help keep the throat open during rest by bringing the jaw forward, also helping relieve snoring.
- Surgery. If treatment hasn’t eased your sleep disorder for more than three months or in more severe cases, surgery might be the best form of action. Surgeries include:
– Tissue removal or shrinkage
– Jaw repositioning
– Implants
– Nerve stimulation
– Tracheostomy (creating a new air passageway)
– Tonsil removal
Treating sleep apnea may be as simple as making healthy lifestyle changes. Talk to your provider to determine the best treatment plan for you.
Using over-the-counter and prescription sedation medications puts you at a higher risk of developing sleep apnea.
Is Sleep Apnea Preventable?
There is no direct approach to prevent sleep apnea, but we have tips for you to follow to reduce the likelihood, such as:
- Stay active. The best way to reduce the risk of sleep apnea is to reach and maintain a healthy weight. Working out a few days a week can make a significant difference and help lessen symptoms.
- Practice good sleep hygiene. Using over-the-counter and prescription sedation medications puts you at a higher risk of developing sleep apnea.
- Maintain existing health conditions. High blood pressure, high cholesterol, and diabetes are key factors that exacerbate sleep disorders.
- Limit alcohol consumption. Consuming alcohol multiple times a week slows down breathing (even if you’re in shape). You don’t have to completely eliminate alcohol, but reducing the amount consumed is worth consideration.
- Regular checkups. Visit your doctor at least once a year for an annual exam to ensure your health is on the right track.

What Is the Correlation Between Dentistry and Sleep Apnea?
Patients tend to visit their dentists more regularly than their doctors, so they are usually the first providers to recognize the signs of sleep apnea. Bruxism (teeth grinding) is one of the initial signs of this condition. You might experience dental symptoms that are directly related to sleep apnea, such as:
- Cracked, broken, or missing teeth
- Excessive teeth grinding or jaw clenching
- Worn front teeth
- Pain when chewing
- Chronic headaches
- Neck and shoulder pain
At Asheville Dental, we offer a comfortable alternative to those suffering from sleep apnea and other sleep disorders. We can help provide the best lifestyle recommendations and comfortable oral devices that aid you in getting a peaceful night’s sleep. If you have questions about sleep apnea, call us today for a free consultation!





